By Paula Oldeg, MD, CCHP
Vaccine efficacy is supported by extensive evidence demonstrating substantial reductions in morbidity and mortality across multiple diseases and populations. Vaccines are paramount in reducing hospitalizations and community transmission and for containing outbreaks.
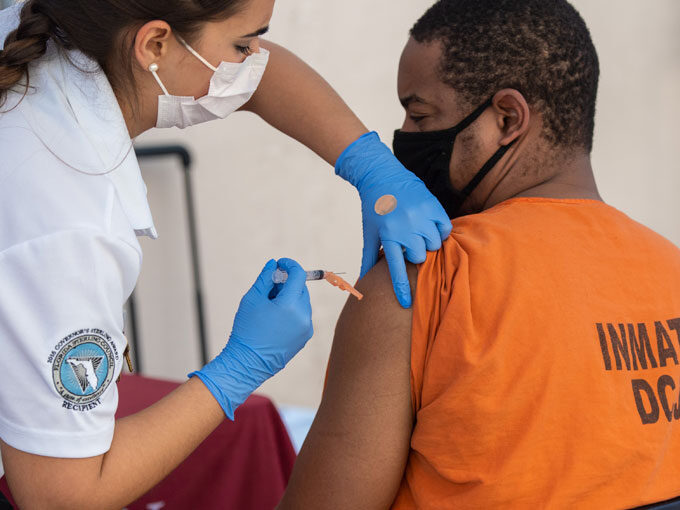
Justice-involved individuals in particular stand to benefit from comprehensive vaccine programs. The incarcerated patient is at higher risk of acquiring communicable diseases than the average person due to facility-related factors such as crowding and high turnover rates, and individual factors including chronic disease, substance use, and mental illness. Incarcerated patients often cannot self-isolate or otherwise protect themselves as they would in the community.
Vaccines provide protections through direct effects (individual protections) and community effects (herd immunity). Data show that when vaccines are given to incarcerated populations, the vaccines perform comparably to the general population and protect both vaccinated and unvaccinated individuals.
Vaccination can mitigate outbreaks in both the facility and the community and also contributes to disease containment. Awareness of postexposure strategies are pertinent for correctional health care professionals, as measles outbreaks are currently ongoing at detention facilities in Texas. Administrating the measles vaccine within 72 hours of exposure has estimated effectiveness for the prevention of measles ranging from 83% to 100%, according to a recent study in The New England Journal of Medicine. Corrections-based vaccine programs have additionally played a role in mitigating community outbreaks of hepatitis A and COVID.
Influenza, COVID-19, and RSV vaccines are markedly effective in reducing serious illness and hospitalizations. Despite the significant seasonal variation of influenza, vaccination provides protection against severe outcomes. A 2025 meta-analysis found vaccine effectiveness of 42% against hospitalization, 51% against pneumonia, 52% against ICU admission, and 55% against ventilatory support. COVID-19 vaccines demonstrate excellent protection against severe disease. A Cochrane review found vaccines result in large reductions in severe or critical COVID-19, ranging from 76% to 98%. RSV vaccines are recommended for older adults (age >75 and age >60 for high-risk individuals). Recent data show vaccines provide 77 % protection against RSV-associated lower respiratory tract illness and 83% effectiveness against RSV-related hospitalization in adults aged 60 and older.
What Should You Do? Vaccine Strategies
NCCHC has incorporated guidelines related to seasonal and indicated vaccinations into Standard B-03 Clinical Preventive Services of its 2026 jail and prison Standards. As COVID is now part of the respiratory virus landscape rather than a standalone novel condition, NCCHC has removed the position statement specifically related to COVID vaccines. Per the standard, at minimum, facilities should give strong consideration to administering seasonal influenza vaccinations to high-risk populations. The correctional facility’s responsible physician should develop and approve an evidence-based vaccination program for the patient population while carefully reviewing vaccine recommendations from public health authorities and professional health associations.
The greatest challenge is achieving adequate vaccine coverage, which can be complicated by vaccine hesitancy, transfers between facilities, and release before vaccine series completion.
Strategies to improve uptake include offering vaccines within one month of entry, active outreach by health workers, accelerated dosing schedules for short-term incarceration, and education efforts.
Patient education should promote health literacy for patients, emphasizing the importance of vaccines as a preventive and potentially lifesaving intervention. The proven benefits and potential risks of each vaccination should be reviewed and patients’ questions and concerns thoughtfully addressed by health educators.
The NCCHC standards support vaccines as a key link in disease prevention and containment to aid in maintaining a healthy space for all—patients, health staff, custody partners, and the community at large.
Paula Oldeg, MD, CCHP, is medical director at the Buzz Westfall Justice Center in Missouri. She is the American College of Emergency Physicians liaison to the NCCHC Board of Representatives and a member of the Policy and Research Committee.
References
- Archer, H., McCoy, S. I., Sears, D., Kwan, A., Kuersten, M., Lewnard, J. A., & Bertozzi, S. M. (2024). Indirect vaccine effectiveness in an outbreak of Alpha B.1.1.7 variant in a California state prison, May 2021. Vaccine, 42(12), 3057–3065. https://doi.org/10.1016/j.vaccine.2024.03.062
- Chin, E. T., Leidner, D., Zhang, Y., et al. (2022). Effectiveness of coronavirus disease 2019 (COVID-19) vaccines among incarcerated people in California state prisons: Retrospective cohort study. Clinical Infectious Diseases, 75(1).
- Graña, C., Ghosn, L., Evrenoglou, T., Jarde, A., Minozzi, S., Bergman, H., Buckley, B. S., Probyn, K., Villanueva, G., Henschke, N., Bonnet, H., Assi, R., Menon, S., Marti, M., Devane, D., Mallon, P., Lelievre, J. D., Askie, L. M., Kredo, T., Ferrand, G., Davidson, M., Riveros, C., Tovey, D., Meerpohl, J. J., Grasselli, G., Rada, G., Hróbjartsson, A., Ravaud, P., Chaimani, A., & Boutron, I. (2022). Efficacy and safety of COVID-19 vaccines. Cochrane Database of Systematic Reviews, 12(12), CD015477.
- Ha Do, L. A., & Mulholland, K. (2025). Measles 2025. The New England Journal of Medicine, 393(24). https://doi.org/10.1056/NEJMra2504516
- Lassen, M. C. H., Højbjerg, N. D., Christensen, S. H., et al. (2026). RSV prefusion F vaccine for prevention of hospitalization in older adults. The New England Journal of Medicine, 394(2), 138–151. https://doi.org/10.1056/NEJMoa2509810
- McCarthy, C. V., O’Mara, O., van Leeuwen, E., CMMID COVID-19 Working Group, Jit, M., & Sandmann, F. (2022). The impact of COVID-19 vaccination in prisons in England and Wales: A metapopulation model. BMC Public Health, 22(1), 1003.
- National Commission on Correctional Health Care. (2026). Standards for health services in jails.
- Nelson, N. P., Weng, M. K., Hofmeister, M. G., et al. (2020). Prevention of hepatitis A virus infection in the United States: Recommendations of the Advisory Committee on Immunization Practices. MMWR Recommendations and Reports.
- Saif-Ur-Rahman, K. M., King, C., Whelan, S. O., Blair, M., Donohue, S., Madden, C., Kothari, K., Sommer, I., Harder, T., Dauby, N., Moustsen-Helms, I. R., Ruta, S., Frère, J., Schönfeld, V., Poukka, E., Lutsar, I., Olsson, K., Melidou, A., Adel Ali, K., Dwan, K., & Devane, D. (2025). Efficacy and safety of respiratory syncytial virus vaccines. Cochrane Database of Systematic Reviews, 9(9), CD016131. https://doi.org/10.1002/14651858.CD016131
- Scientific American. (n.d.). Measles outbreak erupts in one of U.S.’s largest ICE detention centers. Retrieved April 1, 2026, from https://www.scientificamerican.com/article/measles-outbreak-erupts-in-one-of-u-s-s-largest-ice-detention-centers/
- Shattock, A. J., Johnson, H. C., et al. (2024). Contribution of vaccination to improved survival and health: Modelling 50 years of the Expanded Programme on Immunization. The Lancet, 403(10441), 2307–2316.
- Vicente-Alcalde, N., Ruescas-Escolano, E., Harboe, Z. B., & Tuells, J. (2020). Vaccination coverage among prisoners: A systematic review. International Journal of Environmental Research and Public Health, 17(20), 7589.
- Yegorov, S., Patel, O. D., Sharma, H., Khan, T., Gupta, R., Yao, M., Sritharan, A., Silverman, N., Pullenayegum, E., Miller, M. S., & Loeb, M. (2026). Effectiveness of influenza vaccination to prevent severe disease: A systematic review and meta-analysis of test-negative design studies. Clinical Microbiology and Infection, 32(2), 219–229. https://doi.org/10.1016/j.cmi.2025.09.023
- Wilder-Smith, A., Longini, I., Zuber, P. L., Bärnighausen, T., Edmunds, W. J., Dean, N., Spicher, V. M., Benissa, M. R., & Gessner, B. D. (2017). The public health value of vaccines beyond efficacy: methods, measures and outcomes. BMC medicine, 15(1), 138. https://doi.org/10.1186/s12916-017-0911-8